|
Errors in keratometric measurements are responsible for about 10% of refractive errors after cataract surgery. 5 One of the most important parameters in calculating lens power is keratometry. 4Ī non-contact optical biometry remains the gold standard for measuring intraocular lens power before cataract surgery. A significant postoperative refractive error is defined as the difference between the expected and actual spherical equivalent of postoperative refraction above 1.0 D. 3 Competition between centers and increasingly higher patient expectations cause the need to optimize this procedure and systematically reduce the refractive error rate. 1, 2 It is estimated that 7 million such procedures are performed per year in Europe and 20 million worldwide. The results unanimously indicate that refractive errors can be reduced by proper treatment of DED before cataract surgery.Ĭataract removal surgery is one of the most commonly performed eye surgeries. The refractive error was significantly lower after treatment in all studies. Various substances have been used to treat dry eye, such as cyclosporin A, liftitegrast, and loteprednol. In all studies, biometry was performed before and after dry eye treatment, and the mean absolute error was compared. Four clinical studies evaluating the effect of DED on refractive errors were included. PubMed database was searched for keywords: cataract surgery, dry eye disease, refractive error, refractive outcomes, keratometry, and biometry. The purpose of this study is to evaluate the effect of DED on biometric measurements before cataract surgery and postoperative refractive errors. DED also significantly disturbs preoperative biometric measurements, mainly by changes in keratometry measurements. Numerous reports confirm an increase in dry eye symptoms after cataract surgery. It tends to cause a combination of symptoms from the other three types of uveitis.Dry eye disease (DED) is a multifactorial ocular surface disorder characterized by loss of tear film homeostasis with associated ocular symptoms, like dryness, foreign body sensation, and inflammation. Panuveitis is characterized by inflammation in all three layers of your uvea. It tends to be more serious than iritis, but is also the least common form of uveitis. Posterior uveitis affects your choroid that contains blood vessels that supply blood to the back of your eye. Intermediate uveitis causes inflammation of the ciliary body and the vitreous fluid inside your eye. 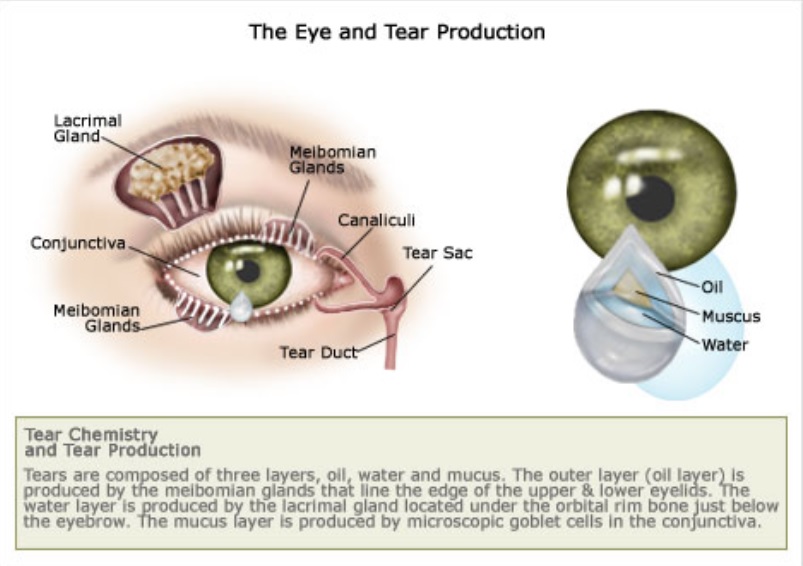
The other three types of uveitis include the following: Intermediate uveitis It’s called recurrent iritis if it returns repeatedly. 
Iritis is called acute iritis if it lasts a short time and chronic iritis if it lasts a long time. It primarily affects people ages 20 to 60 and makes up about 50 to 70 percent of all uveitis cases. Iritis tends to be the mildest type of uveitis and often occurs in otherwise healthy people. When your iris and the space in front of your iris are affected, the inflammation is called iritis or anterior uveitis. Inflammation of your uvea is called uveitis. 
A thin layer of tissue between your sclera and retina (the light-sensitive tissue at the back of the eye). A ring of muscle behind your iris that changes the shape of your lens when you focus your eye. The pigmented and colored part of your eye. The uvea contains the following structures: Your uvea is the middle layer of your eye beneath your cornea and sclera (the white part of your eye). Share on Pinterest Print Illustration by Maya Chastain
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
